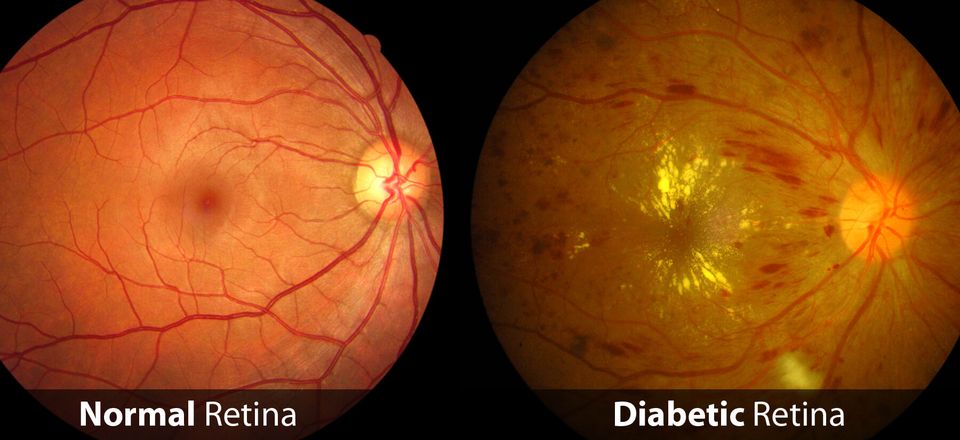
A Complication of Diabetes Involving Abnormal Blood Vessels Which Nourish the Retina of the Eye
Diabetic retinopathy is the leading cause of blindness among adults. Approximately, 25% of current diabetics have some form of the disease. The risk of developing diabetic retinopathy increases with the age of the diabetic person and the duration of the disease. It is estimated that 90% of diabetics may experience some form of diabetic retinopathy over the course of their life. However, only a small percentage of those developing diabetic retinopathy have serious vision problems and even a smaller percentage become blind.
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes mellitus which causes abnormalities in the tiny blood vessels nourishing the retina. These vessels weaken, leak fluid and blood, and fail to provide nutrients necessary for good health in the retina. Left untreated, diabetic retinopathy can result in severe visual loss, including blindness.
What is the retina?
The retina is a thin layer of delicate nerve tissue which lines the back portion of the eye. Light enters the eye and is focused by the lens through the transparent gel-like fluid (vitreous) onto the retina. The retina then changes the image into electric impulses which are carried to the brain by the optic nerve.
The retina has two main parts — the macula and the peripheral retina. The macula is located in the middle portion of the retina close to the optic nerve. The macula is responsible for central vision and color vision. The peripheral retina is the outer region of the retina and is responsible for side vision, as well as night vision.
What is background diabetic retinopathy?
Diabetic retinopathy can take two forms, background retinopathy and proliferative retinopathy. During the early stage of the disease (background retinopathy), small blood vessels in the retina leak a clear fluid (serum) into the surrounding tissue which causes swelling. Abnormal blood vessels may also hemorrhage or leak fats and proteins which form deposits. If fluid collects in the macula, diminished or blurred vision will result. However, if leakage or deposits occur in the outer edges of the retina, no symptoms may be noticed.
Sight is not usually seriously affected in cases of background retinopathy In fact, the condition does not progress in 80% of patients. However, background retinopathy is a warning sign and can progress into the more serious stage of the disease, proliferative retinopathy.
What is proliferative diabetic retinopathy?
Proliferative diabetic retinopathy is the more advanced stage of the disease. New abnormal blood vessels grow over the retina and may grow into the clear vitreous. These new vessels bleed into the vitreous, blocking light from reaching the retina and causing vision to become cloudy. Connective tissue growing along with abnormal blood vessels may contract, pulling the retina off its underlying structures and toward the vitreous (retinal detachment).
Proliferative retinopathy affects approximately 5% of all diabetics and becomes more likely with increased duration of diabetes. If left untreated, proliferative retinopathy can lead to blindness.
What causes diabetic retinopathy?
The cause of diabetic retinopathy is not completely understood. However, it is known that diabetes weakens small blood vessels in various areas of the body, including the retina. Unfortunately, the development of diabetic retinopathy cannot be prevented.
What are the symptoms of diabetic retinopathy?
Though vision may gradually become blurred, significant loss of sight does not usually occur with background retinopathy. Since the patient does not experience pain or external symptoms such as bloodshot eyes or discharge, changes in the retina can go unnoticed unless detected by an eye examination.
When bleeding occurs in proliferative retinopathy, the patient has clouding or complete loss of sight. Connective tissue pulling on the retina causes distortion and blurring. However, if abnormalities occur in the peripheral retina, the patient may not experience any symptoms.
How is diabetic retinopathy diagnosed?
A comprehensive eye examination is the best protection against the progression of diabetic retinopathy. The disease can be detected by viewing the retina with instruments which illuminate and magnify the structures of the eye. If diabetic retinopathy is found, fluorescein angiography is performed to determine the extent of blood vessel leakage. In this procedure, a series of photographs are taken as a dye travels through the retinal vessels. In some cases, ultrasound equipment may be used to check for retinal detachment.
How is diabetic retinopathy treated?
Treatment of diabetic retinopathy depends on the location of the disease and the degree of damage to the retina. If retinopathy occurs in the peripheral retina, careful monitoring of the disease may be all that is necessary. When retinopathy affects the macula and central vision, laser treatment is usually necessary. In cases of background diabetic retinopathy, lasers may be used to seal blood vessels that have leaked serum. Laser treatment may not halt the disease entirely but can reduce further visual loss by delaying the onset of proliferative retinopathy. The proliferative stage of the disease is also treated with lasers to curtail the growth of new abnormal blood vessels.
Laser treatment of diabetic retinopathy is usually done on an outpatient basis in an office or outpatient center.
Laser surgery is a safe and effective method of slowing or halting visual loss associated with diabetic retinopathy.
Prevention is the best medicine
Early detection and management of diabetic retinopathy is important to arrest or slow the development of the more sight damaging stages of the disease. Even when no symptoms are noticed, the diabetic patient should have frequent eye examinations, as recommended by their doctor. Nondiabetics should also have their eyes examined periodically to help detect the presence of diabetes and other diseases. With careful monitoring, treatment of diabetic retinopathy can usually be started before sight is affected.
If you are experiencing the symptoms of diabetic retinopathy or other vision problems, you should obtain a complete eye examination. If you have diabetes mellitus, you should have a dilated eye examination at least once a year for the rest of your life.
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes mellitus which causes abnormalities in the tiny blood vessels nourishing the retina. These vessels weaken, leak fluid and blood, and fail to provide nutrients necessary for good health in the retina. Left untreated, diabetic retinopathy can result in severe visual loss, including blindness.
What is the retina?
The retina is a thin layer of delicate nerve tissue which lines the back portion of the eye. Light enters the eye and is focused by the lens through the transparent gel-like fluid (vitreous) onto the retina. The retina then changes the image into electric impulses which are carried to the brain by the optic nerve.
The retina has two main parts — the macula and the peripheral retina. The macula is located in the middle portion of the retina close to the optic nerve. The macula is responsible for central vision and color vision. The peripheral retina is the outer region of the retina and is responsible for side vision, as well as night vision.
What is background diabetic retinopathy?
Diabetic retinopathy can take two forms, background retinopathy and proliferative retinopathy. During the early stage of the disease (background retinopathy), small blood vessels in the retina leak a clear fluid (serum) into the surrounding tissue which causes swelling. Abnormal blood vessels may also hemorrhage or leak fats and proteins which form deposits. If fluid collects in the macula, diminished or blurred vision will result. However, if leakage or deposits occur in the outer edges of the retina, no symptoms may be noticed.
Sight is not usually seriously affected in cases of background retinopathy In fact, the condition does not progress in 80% of patients. However, background retinopathy is a warning sign and can progress into the more serious stage of the disease, proliferative retinopathy.
What is proliferative diabetic retinopathy?
Proliferative diabetic retinopathy is the more advanced stage of the disease. New abnormal blood vessels grow over the retina and may grow into the clear vitreous. These new vessels bleed into the vitreous, blocking light from reaching the retina and causing vision to become cloudy. Connective tissue growing along with abnormal blood vessels may contract, pulling the retina off its underlying structures and toward the vitreous (retinal detachment).
Proliferative retinopathy affects approximately 5% of all diabetics and becomes more likely with increased duration of diabetes. If left untreated, proliferative retinopathy can lead to blindness.
What causes diabetic retinopathy?
The cause of diabetic retinopathy is not completely understood. However, it is known that diabetes weakens small blood vessels in various areas of the body, including the retina. Unfortunately, the development of diabetic retinopathy cannot be prevented.
What are the symptoms of diabetic retinopathy?
Though vision may gradually become blurred, significant loss of sight does not usually occur with background retinopathy. Since the patient does not experience pain or external symptoms such as bloodshot eyes or discharge, changes in the retina can go unnoticed unless detected by an eye examination.
When bleeding occurs in proliferative retinopathy, the patient has clouding or complete loss of sight. Connective tissue pulling on the retina causes distortion and blurring. However, if abnormalities occur in the peripheral retina, the patient may not experience any symptoms.
How is diabetic retinopathy diagnosed?
A comprehensive eye examination is the best protection against the progression of diabetic retinopathy. The disease can be detected by viewing the retina with instruments which illuminate and magnify the structures of the eye. If diabetic retinopathy is found, fluorescein angiography is performed to determine the extent of blood vessel leakage. In this procedure, a series of photographs are taken as a dye travels through the retinal vessels. In some cases, ultrasound equipment may be used to check for retinal detachment.
How is diabetic retinopathy treated?
Treatment of diabetic retinopathy depends on the location of the disease and the degree of damage to the retina. If retinopathy occurs in the peripheral retina, careful monitoring of the disease may be all that is necessary. When retinopathy affects the macula and central vision, laser treatment is usually necessary. In cases of background diabetic retinopathy, lasers may be used to seal blood vessels that have leaked serum. Laser treatment may not halt the disease entirely but can reduce further visual loss by delaying the onset of proliferative retinopathy. The proliferative stage of the disease is also treated with lasers to curtail the growth of new abnormal blood vessels.
Laser treatment of diabetic retinopathy is usually done on an outpatient basis in an office or outpatient center.
Laser surgery is a safe and effective method of slowing or halting visual loss associated with diabetic retinopathy.
Prevention is the best medicine
Early detection and management of diabetic retinopathy is important to arrest or slow the development of the more sight damaging stages of the disease. Even when no symptoms are noticed, the diabetic patient should have frequent eye examinations, as recommended by their doctor. Nondiabetics should also have their eyes examined periodically to help detect the presence of diabetes and other diseases. With careful monitoring, treatment of diabetic retinopathy can usually be started before sight is affected.
If you are experiencing the symptoms of diabetic retinopathy or other vision problems, you should obtain a complete eye examination. If you have diabetes mellitus, you should have a dilated eye examination at least once a year for the rest of your life.
